In the dusty outskirts of Vientiane, young motorbike riders roar down a ruler-straight road that stretches for 6km out of the city toward the Thai border. There are no traffic lights or roundabouts to slow them down, and the bikes reach rapid speeds that contrast with the otherwise sleepy nature of Laos’ capital.
Sebastien Perret, a co-founder of the volunteer emergency service Vientiane Rescue, tuts disapprovingly at the sight. As wealth in the city has begun piling up, so has the number of accidents – increasing numbers of people own cars and motorbikes, and the trifecta of problematic drink driving, sporadic enforcement of road rules and few people wearing helmets combine with speed to produce often fatal results.
On a recent evening shift, Perret and his team mill around an old cargo container on the roadside, which has been converted into a makeshift ambulance station. It’s a bare bones operation. There are cracks in the wall, the bunk beds that volunteers sleep in during shifts are spartan and, naturally, it’s cramped.
Perret refers to the reckless petrolheads as “future customers”, but in reality, none of the traffic accident victims picked up has to pay for the service from Vientiane Rescue, whose members attend about 700 incidents each month from four stations dotted across the city. Roughly 270 members volunteer their time, many working through the night after their jobs or schooling are complete for the day. The entire operation runs on a shoestring budget of about $5,000 per month.
“What amazes me the most is not the people we pick up on the street, but the way we do it,” Perret tells me. “It is special. And our volunteers, wow. They are the best people I ever met in my life.”
Vientiane Rescue exists for one simple reason: there is no government-run emergency service in the Laos capital. And, although it may seem unusual at first glance, it’s not the only such service operating in the region’s developing countries.
In Bangkok, where the population is dense and resources are stretched, volunteers are sent out as first responders to accidents, providing basic first aid ahead of the arrival of fully equipped ambulances. Even wealthy Singapore, which has one of the best healthcare systems in the world, runs its free ambulance service off the back of the Singapore Civil Defence Service, staffed by citizens fulfilling the country’s mandatory national service.
Ambulances and emergency services are just one of the major gaps remaining in the region’s public health systems. Although there are vast differences between the quality of healthcare provision in, say, Malaysia and Myanmar, public healthcare is generally deeply underfunded. According to the World Health Organisation, Southeast Asian governments contribute an average of 4% of GDP to healthcare funding, compared to roughly 12% for affluent members of the Organisation for Economic Cooperation and Development, from New Zealand to Norway and Chile to the Czech Republic.
But it’s not just NGOs filling those gaps: private firms are also in on the act. “While much of Southeast Asia’s public healthcare sector struggles with growth and funding issues, the region’s private healthcare market continues to enjoy solid growth, especially in the more developed areas such as Singapore, Malaysia and Thailand,” international professional services firm Deloitte says in its 2015 Healthcare Outlook report for the region.
According to global research and consultancy firm Frost & Sullivan, the value of the region’s healthcare market is set to reach $150 billion this year. Business strategy consultancy LEK says in its report Private Healthcare Providers in Southeast Asia: Poised for Continued Growth that a range of factors, not least among them growing wealth, are contributing to rising demand for quality healthcare. “Sustained economic development in Southeast Asia has led to a rise in incomes, increasing the consumer base of those who are willing to pay for healthcare,” it says.
This is not only taking place in more established markets, but also in developing countries such as Laos, Cambodia and Myanmar, where emergency healthcare services are an increasingly integral part of private providers’ business models.
One private healthcare provider hoping to capitalise on this demand is the shiny new $35m Sunrise Japan Hospital, which opened on Phnom Penh’s Chroy Changvar peninsula last September. Cambodia’s shaky healthcare system has long inspired middle- and upper-income patients to travel overseas for treatment – to Vietnam, Thailand or Singapore, depending on an upwards-sliding scale of means.

Dr Takehiro Kozuma, the deputy clinic director at Sunrise Japan, says the hospital, which specialises in neurosurgery and stroke care, wants to encourage more Cambodians to stay closer to home when they fall ill. The emergency department is a key to its operations: the hospital has 120 staff, 20 of whom work in emergency, and it has invested $75,000 in an ambulance, with plans to purchase a second vehicle.
“[For] some patients, for example stroke patients, time is very important. If patients go abroad, their condition can get worse,” Kozuma says of emergencies. “Also, patients pay money to other [overseas] countries, so we want to save money and save lives in Cambodia.”
The hospital, which was established in a partnership between three Japanese companies, is trading on its affiliation with Japan, a country respected locally and internationally for the quality of its healthcare. There are five Japanese doctors working at the 50-bed hospital, while all the Cambodian medical staff have undergone training in Japan.
This is an important selling point for emergency medical service providers as, according to Akiko Sasaki, the country director of Japanese non-profit Side by Side International, “many people don’t trust medical skills [and] treatment in Cambodia”. Private emergency ambulance services have gained a particularly bad reputation, with disreputable private clinics fighting to arrive on the scene of traffic accidents before the public service (a phenomenon the government has outlawed but ambulance drivers say persists). Meanwhile, the public service, which is heavily supported by Side By Side – it has donated more than 35 ambulances as well as a slew of vehicles that have been converted – is often criticised for being slow to reach victims.
Affiliations with international healthcare providers are a common theme among the more upscale hospitals that have opened in Phnom Penh in recent years. Others include Royal Phnom Penh Hospital on Russian Boulevard, which is managed by Bangkok Hospitals Group, and Cho Ray Phnom Penh Hospital in Chbar Ampov district, a branch of its namesake in Ho Chi Minh City.
Each takes a different approach again to ambulance services: Cho Ray is among a number of Cambodia-based hospitals that transport seriously ill patients by road to Vietnam for treatment – a journey that can take five to six hours – while Royal Phnom Penh offers air evacuations to Bangkok for those who require specialised treatment – and can afford the price. In general, the former service costs hundreds of dollars, while the latter can run into the thousands.
These glossy, well-equipped outfits – the waiting room at Sunrise Japan feels more like the interior of a hotel than a medical institution – stand in stark contrast to Cambodia’s public healthcare providers. At the Khmer-Soviet Friendship Hospital, emergency department chief Dr Sourn Samith takes a break from directing a team of doctors and nurses to give a tour of the facilities.
Private ambulance services provide early intervention, which is possible when you have highly trained emergency doctors who can immediately assess a patient’s health condition in order to employ the right equipment, supply and medicine, bed-to-bed until the patient is transported to a primary care centre”
In one section, a 35-year-old woman suffering a hematoma after she had a stroke lies in a coma, awaiting transfer to the ICU for surgery. “She was transported by ambulance,” he says, all the way from Prey Veng province, which lies some three hours away. “She had no treatment there. We just started her with oxygen.” A junior doctor is ventilating the patient by hand, her chest rising with each squeeze of his hands. The department does not have a mechanical ventilator.
Most patients cannot afford to pay for their own treatment, although a few are covered by government programmes for the poorest citizens. Dr Samith says they never turn away those who lack funds, but without others making up the shortfall it makes it difficult to pay staff adequately or purchase life-saving equipment. “If we could get more money from patients, we could [provide] support for the staff and especially improve our materials and equipment,” he says.
Sasaki, whose NGO also provides medical equipment to public hospitals in Cambodia, is much more stark in her assessment of the system. “It’s in a very sad state,” she says. It’s a reality that exists throughout the region, according to the 2017 Global Healthcare Outlook report from Deloitte, which described “an increasing gap [in Southeast Asia] between the state-of-the-art hospital and treatment infrastructure in private institutions serving medical tourism and the well-to-do, and the very basic public infrastructure for the local population”.
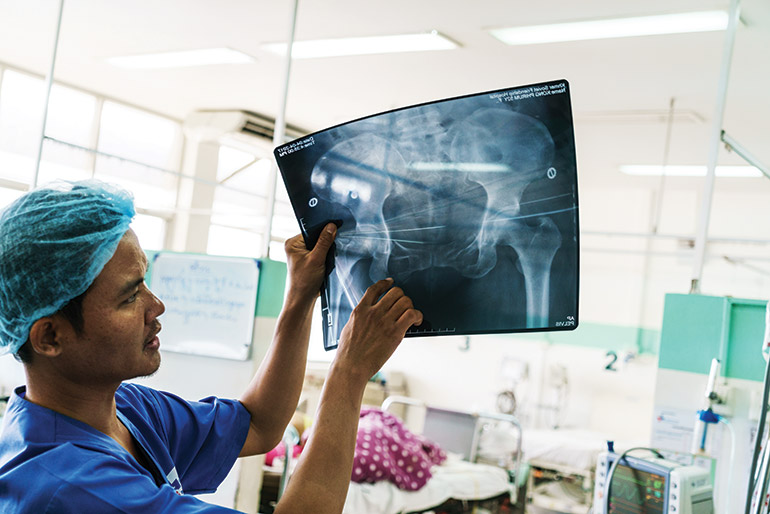
Nevertheless, Robert Tyler, the country manager of global medical provider International SOS Myanmar, argues that private ambulance services are meeting a major need. International SOS treats 9,000 patients a year in Myanmar, with six to eight emergency ambulance callouts a month, in a country that only began introducing public ambulance services in 2015 and has a woefully inadequate hospitals system. Tyler says private operators play an “essential” role across the region in terms of “rapid mobilisation of medical staff, capable to stabilise patients during a life-threatening or limb-threatening injury or illness”.
“Private ambulance services provide early intervention, which is possible when you have highly trained emergency doctors who can immediately assess a patient’s health condition in order to employ the right equipment, supply and medicine, bed-to-bed until the patient is transported to a primary care centre,” he says.
As long as public healthcare in the region’s developing countries languishes below international norms, those with the means to do so will continue turning to private operators who can provide higher standards, causing issues in the public sphere but providing a boon for healthcare businesses.
Dr Samith, who says private operators usually refer patients who cannot pay to the public system, has a straightforward solution of his own in regards to addressing the immense inequities in Cambodia’s healthcare sector: “For the private hospitals, I think they must keep the small place [for providing treatment] to the poor people.”


