Cambodia is an AIDS success story, but Covid-19 risks undermining that
As the world marks World AIDS Day 2020 amidst a novel pandemic, health consultant David Wilkinson warns against complacency as Cambodia's successful fight against HIV/AIDS in recent decades risks coming undone as healthcare is stretched and the economy slows
The dawn of the new decade saw the emergence of a novel virus that jumped to humans from an animal host. The virus quickly and surreptitiously spread across the globe, infecting millions of people and causing high numbers of hospitalisations and deaths.
The initial reaction of some political leaders and large numbers of the general public was denial, followed by anger. Accusations were made against certain countries and ethnic groups, and protesters marched in the streets. The poor, the vulnerable and the marginalised were the least able to cope with the ravages of the disease. Some health experts wondered whether the novel virus could ever be effectively addressed, fearing a future in which infection rates continued to spiral upwards.
The new decade was the 1990s, and the novel virus was the human immunodeficiency virus (HIV), which causes AIDS. There are clear parallels to be drawn between the emergence and spread of HIV in the 1990s and the emergence at the dawn of the present decade of the novel coronavirus (SARS-COV-2), which causes Covid-19.
There are also some key differences. When HIV emerged as a global pandemic, it took years to mobilise an effective response. For Covid-19, the timeframe for the response has been compressed into weeks and months. In the last few days at least three vaccines against Covid-19 are awaiting regulatory approval, and distribution plans are already underway. But even after decades of intensive research, a vaccine against HIV remains elusive.
Cambodia has shown remarkable success in tackling the twin pandemics of AIDS and Covid-19, with the victories in both attributable to a willingness to explore and refine innovative and evidence-based approaches. But as the pandemic strains many of critical interventions that have proved effective in Cambodia’s successful AIDS response in recent decades, many are warning against complacency.
As Dr Vladanka Andreeva, Country Director, UNAIDS Cambodia, told me: “We cannot stop new HIV infections in Cambodia if we stick to business as usual… The Covid-19 crisis is a wake-up call, an opportunity to do things differently, better and together. Putting people at the centre and grounding our responses in science, human rights and gender-responsive approaches are key to ending the colliding pandemics of HIV and Covid-19”.
Key elements of success in the Covid-19 response in Cambodia have included stringent border controls, screening and testing, persistent contact-tracing and isolation, coupled with clear public health messages and strong political support. Some of these measures were learned during the SARS and Avian Influenza epidemics that affected the region, and others are derived from lessons learned during the onset of the AIDS epidemic in Cambodia.
A review in 2006 noted that the HIV/AIDS response in Cambodia had high level political support, was data-driven and used innovative approaches, including condom social marketing, community outreach, contact tracing, harm-reduction, and identifying and responding to changing patterns of sexual behaviour.
In the 1990s, community outreach was an innovative yet untested approach, and proved to be a crucial element of successful HIV prevention efforts. Through its network of community-based organisations (CBOs), Cambodian non-governmental organisation KHANA continues to refine the community outreach approach today.
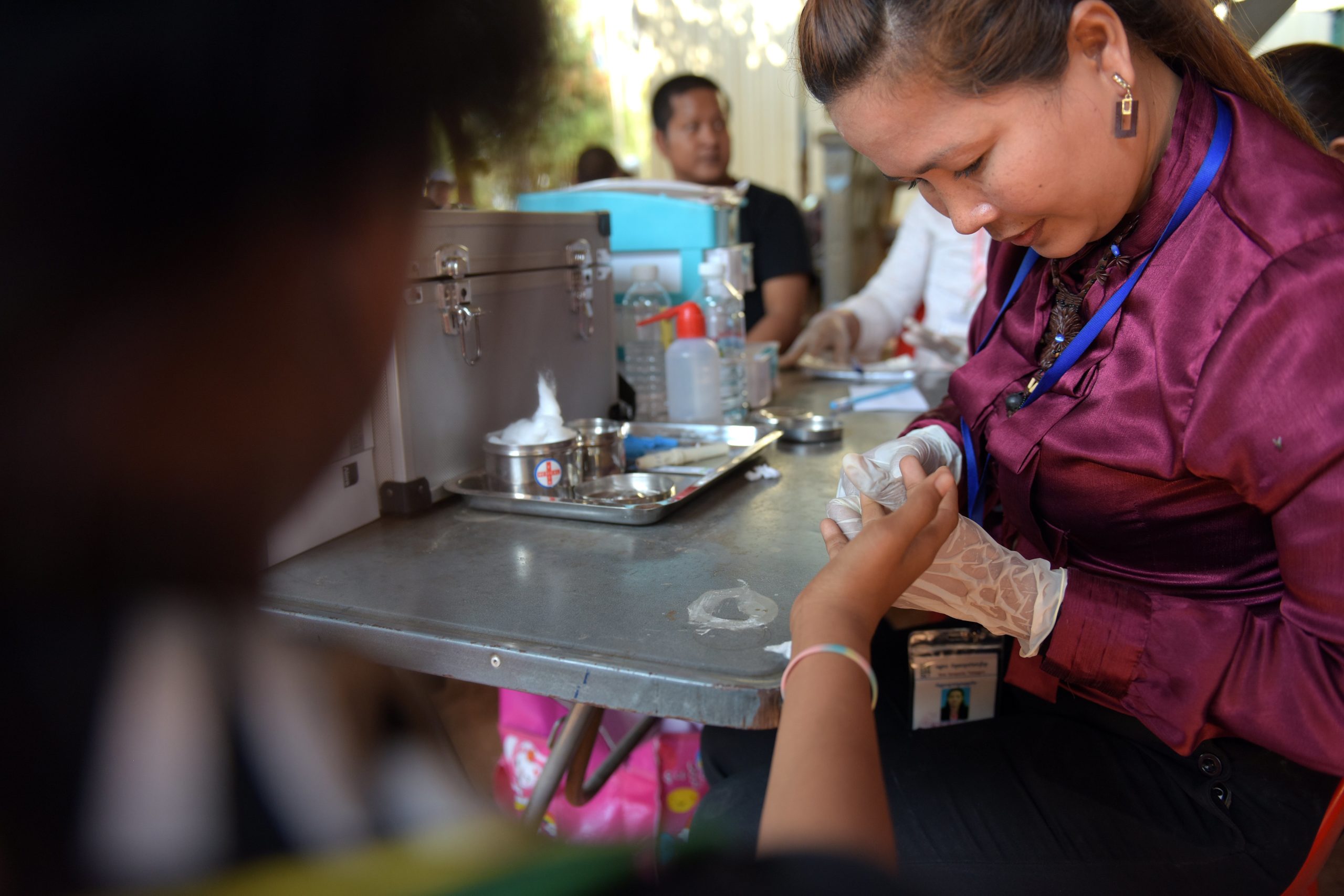
Moeun Kimliang is a university undergraduate. But every weekday evening at 7pm she takes a break from her studies to join her team of seven outreach workers from Cambodian Women for Peace and Development, one of KHANA’s CBOs, and conduct outreach activities at KTVs, karaoke bars and massage parlours and with street-based entertainment women. The team supplies condoms and HIV test kits, provides counseling, and refers those who test positive for HIV to the Chhouk Sar clinic for confirmatory tests and antiretroviral therapy (ART).
Kimliang’s shift ends at 12.30am, and she estimates that her team reaches between 50-60 female entertainment workers each evening, of whom around half accept to be tested for HIV. She notes that when entertainment venues were closed due to Covid-19, many of the female workers returned to their villages, but some turned to street-based entertainment work, which increases their vulnerability.
Cambodia is one of only three Asia-Pacific countries – along with Australia and Thailand – to have successfully met its HIV treatment targets

Chhorm Lonh is a businessman, but after work during the week he joins his team from Men’s Health Cambodia, also a KHANA’s CBO, to conduct outreach work among men who have sex with men (MSM). Some of these meet openly at bars such as Blue Chilli, but others prefer to keep their identities hidden and congregate in groups in ‘safe spaces’, such as parks in Koh Pich, Bang Kak and 60 metre street. Lonh notes that, since the onset of Covid-19 his team is meeting increasing numbers of MSM in these safe spaces and that they are increasingly engaging in high-risk sexual behaviour. The reasons for this are presently unclear, but there is anecdotal evidence that job losses, increased free time and stress may be compounding factors.
A key element in the global AIDS response has been in expanding access to ART to people infected by HIV. By reducing the viral load, ART fulfils the dual role of prevention and treatment, and Cambodia is one of only three Asia-Pacific countries – along with Australia and Thailand – to have successfully met its HIV treatment targets. Of the estimated 73,000 people in Cambodia living with HIV, 84% know their HIV status; of those who know their HIV status, 99.8% of these are accessing ART, and 96% of these have their viral load suppressed.
Cambodia continues to explore innovative approaches to HIV treatment and prevention. A three-year pilot programme of community ART delivery is being trialled by the National Centre for HIV/AIDS, Dermatology and Sexually Transmitted Infections and KHANA to expand access to ART for people infected by HIV.
Under this model, a ‘self-help group leader’ is authorised to collect 3-6 month’s supply of antiretroviral drugs for a cluster of 20 clients who have viral stability and demonstrate good adherence to treatment. If successful, the initiative will be scaled up nationally, thus reducing travel and time costs for people infected by the virus.
While this model already represented a potentially innovative approach to community ART delivery, its value has become even more apparent since the onset of the pandemic.
A recent online survey conducted among people living with HIV revealed that many were fearful about travelling to clinics to collect their anti-retroviral medication because of the perceived risks of contracting Covid-19. The community ART delivery initiative is ensuring continued access to treatment for this vulnerable group, whose immune systems are already compromised by HIV.

While Cambodia has made major strides in tackling the HIV pandemic, challenges remain.
KHANA Executive Director Dr Choub Sok Chamreun notes that “a major challenge faced by the national response is to reach the estimated 11,000 – 12,000 people who don’t know that they are infected with HIV”. Research suggests that the majority of these are men who have sex with men, transgender women, people who inject drugs, people who use drugs and female entertainment workers.
These groups, which are known as ‘key populations’, collectively account for more than two thirds of all new infections in Cambodia. Stigma, discrimination and criminalisation of their behaviours, coupled with a reluctance to disclose their HIV status because they buy or sell sex, means that these populations are ‘hard to reach’ with HIV interventions. Dr Chamreun notes that “some key populations exhibit multiple high-risk behaviours, e.g. they may use or inject drugs, buy and sell sex with multiple partners and not use condoms consistently”.
To help reach the ‘hard-to-reach’, HIV prevention programmes are utilising social media to enhance and expand upon existing outreach approaches. MyCommunity Websites and Facebook pages (SMARTgirl, M.Style and Sreysros) have been set up to reach each of the key populations, as well as a dedicated Voice4U hotline 1295. Interactive approaches are used to build up risk profiles, and interventions are targeted to those screened to have high-risk behaviours.
To reduce the numbers of new infections, especially among key populations, the national HIV programme is expanding access to pre-exposure prophylaxis (PrEP),and estimates that rates of new infections can be reduced by over 90% if users adhere to the treatment.
In order to expand access to HIV testing, the national HIV programme is rolling out HIV self-testing (HIVST). Key populations can request HIVST kits from community outreach workers, or can pick them up confidentially at selected pharmacies and non-governmental organisations. Users collect their own specimens and then perform the HIV test themselves, either alone or with someone they trust. Pre- and post-test counselling is provided for users through educational videos posted on dedicated websites or by scanning a QR code on the package insert.
The Covid-19 pandemic is placing stress on Cambodia’s economy and health system, and how each of us gets through the day. Recent months have shown that the ongoing need for flexibility and innovation in pandemic response – both HIV and Covid-19 – is paramount if Cambodia is to maintain its status as one of the region’s AIDS success stories.
David Wilkinson is a Phnom Penh-based independent consultant in global health.

