Editors Note: While this follow-up on Roka village was first published in print in 2017, the case reentered the news in October 2019 as Cambodia’s Supreme Court upheld the decision of a Battambang court to sentence 60-year-old unlicensed medical practitioner Yem Chrin to 25 years in prison for infecting almost 300 people with HIV in 2014. He had apparently told the court that he reused syringes on multiple patients because he found it difficult to obtain new ones.
In addition to this story, you can also read our 2014 interview with the Nobel Prize-winning virologist Françoise Barré-Sinoussi, jointly credited with discovering HIV, who told the Globe at the time of the Roka village tragedy that Cambodian prime minister Hun Sen had been “misinformed”, after he made public comments saying he did not believe reports of the virus’ outbreak in the village were accurate.
On the outskirts of Cambodia’s Battambang province, down a broken dirt road bleached white by the sun, Prum Ly is waiting within the walls of her hut to die. Outside in the afternoon heat, half-starved chickens scrabble in the dirt, stripped to the skin by some nameless wasting.
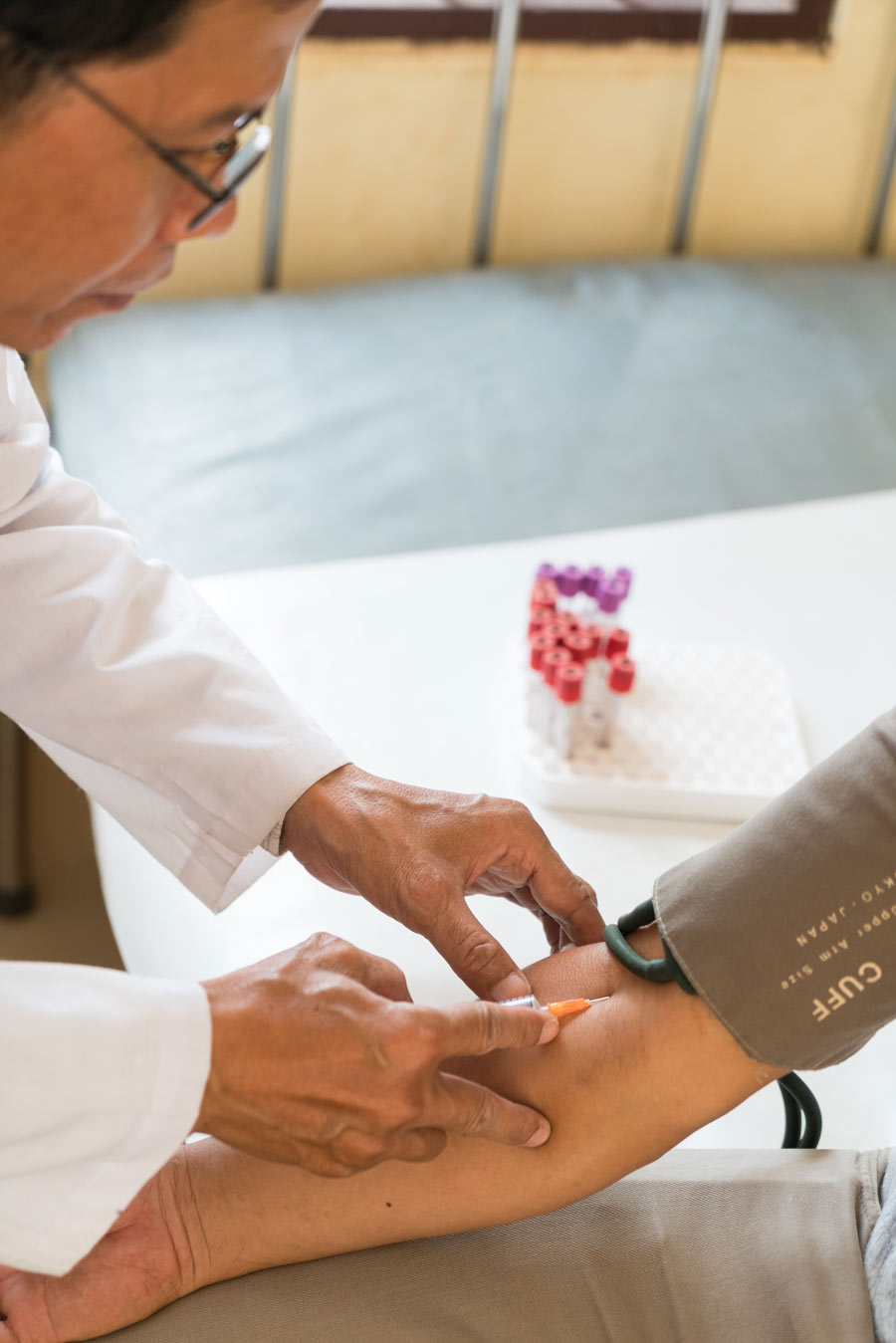
In December 2014, it began to emerge that 292 people in Roka village had been unknowingly infected with HIV by Yem Chrin, an unlicensed medic who treated many families in the area. Today, supported by the Ministry of Health and the Global Fund to Fight Aids, Tuberculosis and Malaria, those infected remain locked in a limbo of monthly medication, tethered to their local health centre through a strict regimen of anti-retrovirals that leaves them listless, sweating and sick.
For 56-year-old Ly, the relentless treatment proved too much. “I only took [the medicine] twice – I fainted,” she says, a shapeless grey jacket hanging off her jutting shoulders. “It was just too bad. I couldn’t take it any more.”
Ly is one of a handful of infected villagers for whom the side effects of HIV treatment have become unbearable. Unable to provide for herself, she depends entirely on the financial support of her eldest son. Her husband, a soldier, died more than 20 years ago.

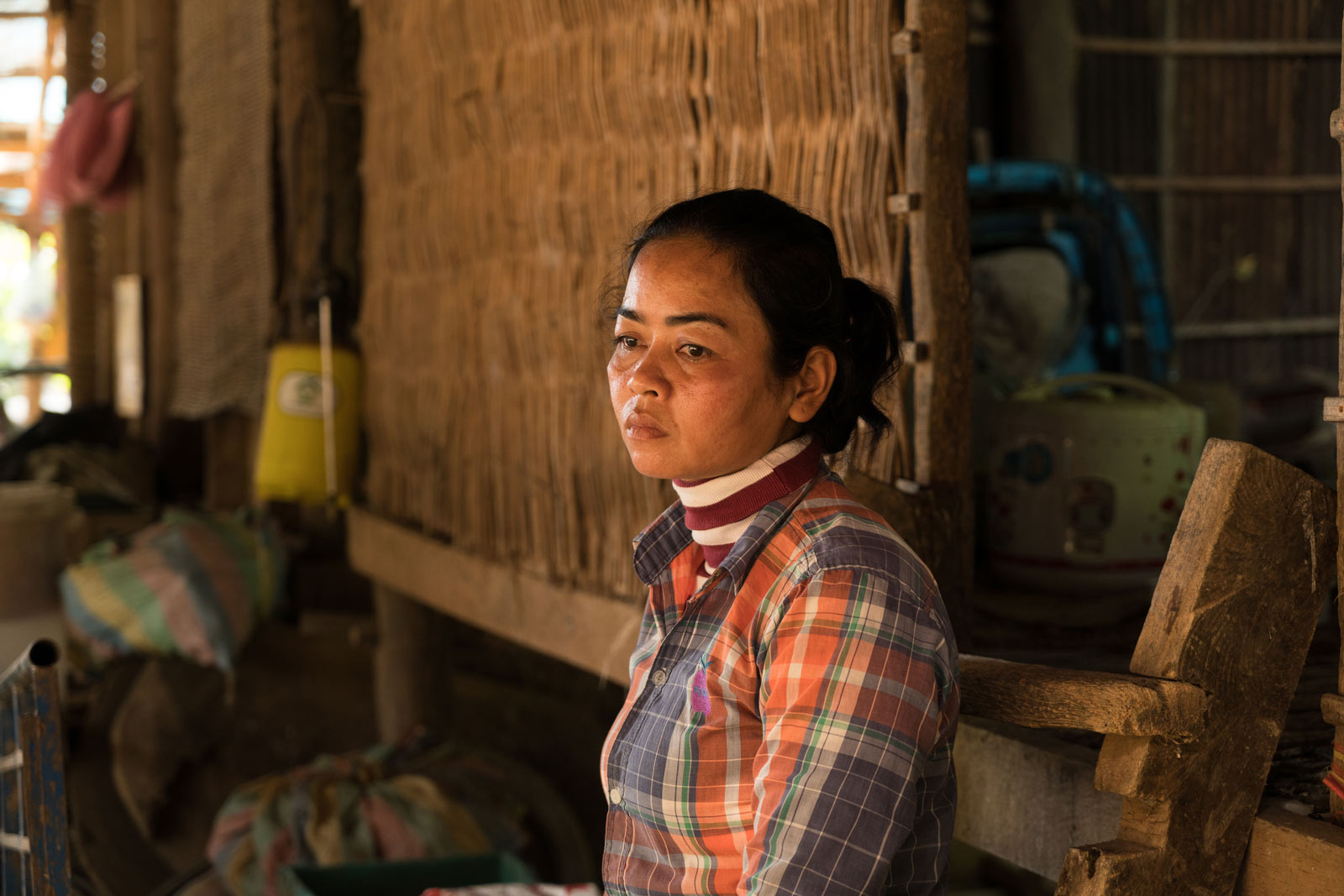
The first time that Soum Saren’s aunt underwent treatment, the nausea was so bad she was admitted to Battambang’s provincial hospital, where she remained for ten days. Unable to take the strain on her ageing body, Saren’s aunt has apparently since refused all treatment despite her family’s pleas.
Saren stares into the red dirt with heavy eyes. Across the wrecked road, the Roka Health Centre squats as a reminder of her aunt’s suffering. “I tried to convince her to take it, but she said she’ll die eventually – with or without the medicine,” she says. Her voice never rises above a whisper.
Roeun Man, a nurse trained in the treatment of HIV, came to Roka Health Centre a little over six months after the outbreak. He said the side effects of the anti-retroviral therapy used to treat HIV could be severe. “The most common side effects here are rash, fever, diarrhoea, headache, and according to what they have told me, some even experienced a burning sensation all over their skin,” he said.
Of the hundreds infected by Chrin’s negligence, 22 are now dead. He is serving a 25-year jail sentence after it was found that he reused contaminated syringes on house calls. The medic’s last victim, the 83-year-old abbot of the local pagoda, succumbed to tuberculosis in early February. Overcome by bouts of nausea from his regimen of anti-retrovirals, Mom Heng had not taken his medication since April.

Buddhism for Development director Heng Monychenda, whose organisation provides counselling and support for those infected with HIV in Roka and the wider Battambang area, said the abbot’s death was a devastating loss for the community.
“He was a very strong person,” Monychenda said. “When he got HIV he tried to take the medicine, but later on he could not bear it. Whenever he took it he started vomiting – he couldn’t eat.”
Man said there had not been any new cases of infection since the initial outbreak but cautioned that people refusing to undergo treatment were potentially putting non-infected villagers in danger.
“They risk infecting their children or other family members – but there’s only a small chance of that happening. But if they have cuts on their bodies, especially when the viruses have weakened them to the last stage, then the chance of infection is higher.”
Even for those who escaped infection, Roka remains a place of poverty and stagnation. Sim Pov, who has been commune chief since 2012, said Roka is crippled by unemployment and poor sanitation.
“Before, we received funding from many sources – government, health ministries, NGOs and Buddhism for Development,” she said. “But this year, we received less.”
Although Pov stressed she was grateful for the support already provided by the government, she said there were few opportunities for people in the community to earn a living for themselves and their families.

“Initially in December 2014 and 2015, there were many sources [of funding] – even from Christian churches,” she said. “But now, even though we have requested more from the government, we don’t get much.”
Ibon Villelabeitia, a communications specialist at the Global Fund to Fight Aids, Tuberculosis and Malaria, told Southeast Asia Globe the reduced funding for Cambodia was due in part to the government playing a more active financial role in the campaign against HIV – though he said the organisation would continue to offer financial support through 2019. He added that Cambodia had cut its adult HIV prevalence by almost 60% over the past ten years, with roughly four out of five adults and children in need believed to be receiving treatment.
“The Cambodian government has steadily increased its annual spending from its domestic resources to HIV, including increasing contributions towards procurement of anti-retroviral therapy and other programme costs,” he wrote in an email. “With an allocation from the Global Fund for HIV of $41.5m over the next three years – in addition to the Cambodian government’s domestic resources for HIV – the Cambodian government will be able to continue the support and treatment of those affected by HIV during this period.”
But Monychenda said there was little evidence of a long-term plan to raise Roka out of its impoverished state. More immediately troubling, he said, was the dwindling support from those organisations that flocked to Roka’s aid in the first days of the crisis.
“There’s less and less funding, absolutely,” he said, looking down at his fingers and smiling wryly. “In the beginning, the name Roka became a [synonym for] curse – the cursed village. Maybe it still is, even now.”
Additional reporting by Hemmunind Hou


